
Covid-19: Which states fared well and why? Examining the role of higher public spending and better management of resources
28, May 2021 | CJP Team
The pandemic while bringing on a sea of tragedies for Indians, has exposed the unpreparedness of callous governments which left people to the mercy of an over-burdened and a structurally weak health system.
While the enormity of the second wave of Covid in India caught the central as well as state governments off guard, the myopic, even authoritarian attitude of the Central government in 2020, taking decisions unilaterally without consulting state governments has made matters worse.
Under the Constitution, health is a state subject and it is for states to build their own capacities and health care systems as they deem fit. However, at times of crises, in the true spirit of federalism, under the National Disaster Management Act (NDMA), 2005, consultation and coordination are key. This has been woefully lacking.
A healthy cooperative spirit honouring the Federal principles of the Indian Constitution would have been in order; setting up an Inter-State Coordination mechanism that was consultative and inclusive. Instead, we had a series of diktats and flip-flops from the Centre. This combined with weakened state health infrastructures left populations reeling.
Some states fared better: How and Why?
- Nos of persons/ Primary Health Centres
- Nos of Govt Doctors/Persons, Population
While putting the onus entirely upon the states in terms of handling the Covid-19 Pandemic is not entirely correct legally speaking, it remains crucial to examine the role played by state governments and how some states have fared better in managing the Covid-19 fallout better than some other states. There are certainly many factors involved here including building of a robust public health care system over the years, building capacity, augmenting and retaining human resources especially medical professionals, maintaining optimum levels of bed to population and doctor to population ratio as also real time management of crisis by administration under the leadership of an able government. More than anything else, making good, efficient and affordable healthcare accessible to the maximum number of Indians, in the most remote areas, is fundamental to democratising the right to health.
Role of state governments
The International Monetary Fund in its latest World Economic Outlook October 2020 has advocated all major economies to allocate adequate resources for healthcare as the near-term policy priority. While availability of hospital beds and health care workers is essential, elaborate and sustained administrative support and additional healthcare expenditure has gained importance in managing a crisis like Covid. Therefore, a simplistic analysis of public health expenditure will not reflect upon a state’s performance in handling Covid.
The second wave/surge of Covid in 2021 caught the Centre as well as States completely not just unawares but showed up Indian authorities for an absence of scientific and rational understanding of a worldwide Pandemic. Worldwide countries and societies experienced a second wave while India carelessly gloated on coming out of the Pandemic. This attitude showed up the unpreparedness of governments and the callous complacency that set in due to a brief dip in cases which was not in tandem with increasing administration of vaccination doses to the maximum population.
Money spent by the state government on health infrastructure, mainly public health care system, may give the government a solid foundation to work on but it is not a sure shot way of handling the crisis. Having a robust public health care system includes infrastructure, a strong referral system as well as adequate human resources, adequate coverage proportionate to the population and so on.
One of the most important strategies to reduce the out-of-pocket expenditure is to strengthen the primary health care system in the state. Health care systems build on a strong comprehensive primary care service acts as a platform which can reduce the health expenditure considerably.
Public Health Activist, Ravi Duggal, wrote in June 2020 in The Hindu Businessline that states that spend more on health care were less affected by the Covid impact.[1] Larger states like Bihar, Uttar Pradesh, Jharkhand, Madhya Pradesh, Odisha, West Bengal, Karnataka, Gujarat, Maharashtra and Punjab turned out to have the weakest primary healthcare system owing to low spending on health care. Says Duggal, two indicators of availability of public health services is the number of government doctors per lakh population and number of persons per Primary Health Centre (PHC). Again, states like Bihar, Uttar Pradesh, Maharashtra, Karnataka, and West Bengal have more than 30,000 persons per PHC and less than the national average of nine government doctors per lakh population. It is not a coincidence that Maharashtra, Karnataka and UP have also allowed privatisation of the health infrastructure.
The data derived from Health Ministry’s National Health Profile, 2019 showed that Kerala had 15 government doctors per lakh population and 42,403 persons per PHC. On another scale, where WHO recommends a doctor patient ratio of 10:10,000 in Kerala it is 16.5 doctors per 10,000.
The data on public health expenditures across states is reflected in a table as below:
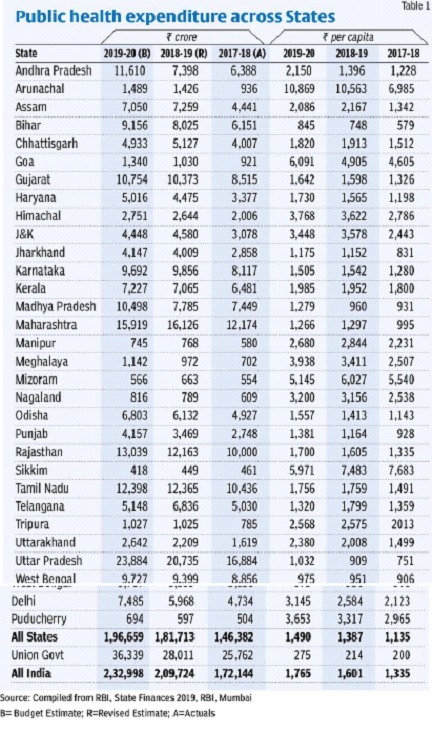
Privatisation of public health care
The NITI Aayog has recommended handing over of district hospitals to the private sector under PPP arrangements as a solution for improving health care system. However, data increasingly suggests that states which have reasonably robust primary healthcare have been able to deal with the Covid first wave, better than the states that did not have a good public health system. Naturally, the same is analogous to higher spending of states on health care out of its GDP and its annual budget. The 2017 National Health Policy recommends 2.5 per cent of GDP or ₹3,800 per capita (at 2017 prices) as the appropriate spending for delivering reasonably good health care predominantly through public health facilities. This translates into ₹5 lakh crore public health spending for the country or 2.5 per cent of GDP or 8.3 per cent of total government budgets.
Privatisation of public health care will only increase out of pocket expenses for people, making health care more and more expensive in the country and out of reach of millions. The example is playing out in reality as governments and courts are having a hard time capping rates charged by private hospitals for Covid treatment. Even in times of such a national health emergency, the private sector sticks to it primary objective – making money. On the other hand, a public health care system has been over burdened and taking on patients unable to afford the sky rocketing private hospital charges.
Almost 62.4% of expenditure on health is borne by households and rest by government. It is well-known that such a high share of out-of-pocket expenses imposes a financial hardship on household budgets and more than often pushes vulnerable households into debt and poverty.
Kerala tops the charts
Kerala has seen the third highest cases in the country following Maharashtra and Karnataka with more than 24.2 lakh cases and over 7,000 deaths – –as per the official count– as of May 24. Mathematicians and data management experts worldwide have projected that India’s deaths could well be three-five times higher than officially admitted figures.
Primary Healthcare Performance Initiative analysed Kerala’s health care reform over the years whereby the state gave local governments control of 35 to 40% of the state budget for improving care and access, regardless of income level, caste, tribe, or gender, reflecting a goal of not just effective but also equitable coverage. The current Public Health Centre (PHC) system consists of sub-centers, primary health centers that support five to six sub-centers and serve a village, and community health centers. Overall, Kerala has maintained low infant and maternal mortality rates, and higher literacy rates, when compared to the national average.[2]
Kerala’s Expert Committee for health submitted a report in 2014 whereby it identified Kerala to have one of the highest ‘out of pocket’ expenditures on health in the country. As per National Health Accounts (2004-05) Kerala had the highest per capita public expenditure as well as highest private expenditure in the country. In its 2020-21 budget, Kerala has allocated 5.5% of its total expenditure on health.
An article in the Huffington Post stated that for over 60 years, Kerala’s health indicators—infant and child mortality rates, birth rates, life expectancy, sex ratio and maternal mortality ratios—have consistently topped the country, despite its middling economic achievements and high unemployment rates.
On May 10, Kerala government fixed a cap on prices that may be charged by private hospitals for Covid treatments. General wards would now cost Rs. 2,645 per day including registration charges, bed charges, nursing and boarding charges, surgeons, anaesthetists, medical practitioner, consultant charges, blood transfusions, oxygen, medicines, pathology and radiology tests and others.With the same facilities, an ICU bed will cost Rs. 7,800 and an ICU bed with a ventilator is capped at Rs.13,800. This move was lauded by the Kerala High Court as well.
Kerala is often described as a state without the urban-rural divide, with civic infrastructure in rural areas being comparable to those in cities. It is also a state with the highest elderly population in the country, with about a fifth of its population over 60.
A report in Al Jazeera from May 11 states that in Kerala and Tamil Nadu, medical oxygen production was augmented and hospital capacities were increased expecting cyclical spikes and troughs of Covid-19 infections. Until late March, Kerala’s case fatality rate (CFR), which is the percentage of deaths to positive coronavirus cases, hovered at 0.32 percent, while in Tamil Nadu, it was 0.52.[3]
However, the state Assembly elections became the hindrance in the continued efforts of the administration to keep Covid spread in check and compelled the newly elected government to enforce a lockdown. Yet, Kerala is one of the few states, which has not faced oxygen shortage until now. In the past year, Petroleum and Explosive Safety Organisation has made concerted efforts to set up oxygen plants and maintain the existing ASU (Air Separation Unit) plants and manufacturing plants both in public and private sectors.[4]
Tamil Nadu
Tamil Nadu has seen 19.4 lakh cases with over 21,000 deaths –as per the official count– as of May 24. Mathematicians and date management experts worldwide have projected that India’s deaths could well be three-five times higher than officially admitted figures.
The State has separate Directorate of Public Health with its own budget. It is staffed by a professional cadre of trained public health managers who are promoted to the Directorate after long years of experience of planning and oversight of public health services in both rural and urban areas.
A study by Swaniti Initiative on Tamil Nadu Public Health System states that apart from having a separate budget for public health in Tamil Nadu, the size of the public health budget is large relative to spending on secondary/tertiary medical care and medical education. The Directorate of Public Health has consistently had larger budgets than the two other Directorates in the Health Department. The state (a) separates the medical officers into the public health and medical tracks, (b) requires those in the public health track to obtain a public health qualification in addition to their medical degree, and (c) orients their work towards managing population-wide health services and primary health care ─ while those in the medical track obtain additional clinical qualifications and are oriented towards providing hospital care.[5]
Tamil Nadu has a Public Health Act, which specifies the legal and administrative structures under which a public health system functions, assigns responsibilities and power to different levels of government and agencies.
A research conducted in 2019 indicated that OOPE per episode of hospitalization in public health centers was lowest in Tamil Nadu (₹2395) and highest in Punjab (₹10540).[6]The Chief Minister Comprehensive Health Insurance Schemes (CMCHIS)cover costs up to ₹5 lacs including quality medical and surgical treatment in public and private health centers. Studies also suggest that good public health care infrastructure, distribution of free medicines, and health insurance for formal sector employees may be the other reasons for low OOPE in Tamil Nadu.[7] While WHO recommends a doctor patient ratio of 10:10,000 in Tamil Nadu it is 19.1 doctors per 10,000.
Tamil Nadu implemented free medicine distribution scheme for all who are utilising public health facilities for treatment since 1995
In its 2020-21 budget, the state has allocated 5.7% of its total expenditure on health. A report in Al Jazeera from May 11 states that in Kerala and Tamil Nadu, medical oxygen production was augmented and hospital capacities were increased expecting cyclical spikes and troughs of Covid-19 infections. Until late March, Kerala’s case fatality rate (CFR), which is the percentage of deaths to positive coronavirus cases, hovered at 0.32 percent, while in Tamil Nadu, it was 0.52.[8]
However, the state Assembly Elections became the hindrance in the continued efforts of the administration to keep Covid spread in check and compelled the newly elected government to enforce a lockdown. Worse, mass election rallies, negative and irresponsible messaging by leaders (giving speeches without wearing masks) caused a rapid spread of the virus. Until April 23, there was sufficient oxygen supply in the state but merely 2 weeks later, the state was facing a shortage of 50 MT of oxygen and the Sterlite plant which was set to open in a week was the faint hope for the state. Chennai has been operating an oxygen war room which functions 24×7 since May 6 with the aim to create a smooth access chain for oxygen for hospitals treating Covid patients in the state.
Odisha
The state has had 7.1 lakh cases as of May 24 and has had about 2,500 deaths – as per the official count—so far. Mathematicians and date management experts worldwide have projected that India’s deaths could well be three-five times higher than officially admitted figures.
Odisha is the second most poor state in India (estimated poverty rate of 32.6%[9]) in the country with a population of over 42 million and a large concentration of scheduled caste and schedule tribe population. Despite high levels of poverty in the state, there have been notable improvements in health outcomes. The state has combated issues like child mortality, maternal mortality over the years.
Political stability in the state has been attributed to political attention towards socio economic development. The per capita spending on health by Odisha government has increased over the years. In 2018 it was Rs.1,143 which increased to Rs.1,413 in 2019 and marginally increased to Rs.1,557 in 2020. It’s not among the highest per capita spends compared to other states where you have north eastern states with way higher expenditure like Arunachal Pradesh (Rs.10,869), Sikkim (Rs.5,971), Mizoram (Rs.5,145) to name a few but it’s definitely more than a few larger states like Maharashtra (Rs.1,266), Uttar Pradesh (Rs.1,032) and Karnataka (Rs.1,505).
Owing to its high poverty levels, the state’s health policy was more focused on an equity based health policy. The Health Equity Strategy (2009–12) aimed to improve the health of the most disadvantaged people in the State, and recognizes the particularly poor health status of Scheduled Tribes and Scheduled Castes and the comparatively poorer districts. The Nutrition Operational Plan (2009–15) aimed to achieve maximum nutritional health of all children below six years of age, especially for the poorest and the most disadvantaged, through effective inter-sectoral coordination.
In Odisha a strong focus of the Health Equity Strategy and the Nutrition Operational Plan was closing the health and nutrition gap between state level outcomes and those of Scheduled Tribes and Scheduled Castes and the underserved KBK+ districts.[10]The Southern belt of 11 districts in the state is known as KBK+ and is made up of the districts of Bolangir, Boudh, Gajapati, Kalahandi, Khandamal, Koraput, Malkangiri, Nabarangpur, Nuapada, Rayagada, and Sonepur.
In Odisha, the underserved and poorer districts in KBK+ have been given special attention including mobile health units which have become the major source of health care in the remote and inaccessible villages. The other efforts include control of malaria related deaths, increasing access of women to health care, posting newly appointed doctors in KBK+ areas and paying them more, increasing institutional deliveries, carrying out surveys to identity out of pocket expenses and so on. This has resulted in reduced gap in ST women and children and others in utilising health care, increased institutional deliveries, progress in reducing number of underweight and stunted children, reducing nutrition disparities in ST children and other social groups and so on.[11]
Odisha was the first state that took proactive steps to ramp up its health care system particularly having a Covid-19 hospital with intensive care units (ICUs) on public–private partnership mode and was among few states to have created a Covid-19 hospital at each district in record time. It also took measures like and setting up a taskforce to oversee the Covid-19 response daily press briefings. These proactive efforts suffered a slight blow when migrants started returning to the various districts across the state in May 2020. Overall, though, it has managed to keep its fatality rate to very low i.e., 0.4%. At present, Odisha has 50 Covid hospitals with maximum number of seven such hospitals in the most affected Ganjam district. Besides, it has built-up 178 Covid care centres and 17,647 temporary medical centres (TMCs). Bulk of these facilities was created as early as May 2020 when number of Covid cases was not so high and by end of May, 2020 it had dedicated Covid health centres in all districts. The government used panchayats and community-based organisations like well-entrenched self-help groups for managing the movement of migrant workers, arranging shelter and running quarantine centres to providing other critical support.
While many states were found struggling in the initial phase of pandemic, Odisha’s long experience of running relief operations during natural disasters has come critical in terms of swiftly organising shelters for migrants and stranded persons during the lockdown. in April, the state empowered sarpanches to ensure quarantine of returnees and their families and all Gram Panchayats (GPs) were allowed to exercise their jurisdictions at the ground level to aid monitoring efforts of the facilities. [12] Odisha has allocated 5.5% of its expenditure for health in 2020-21.
Low public spending = poverty
While public spending on health is an indicator of good human development index, it is also an indicator of poverty. It is largely observed that people get pushed into poverty due to higher out of pocket expenses (OOPE) on health, since that expense is unavoidable and with a weak public health system, people are compelled to shell out money from their pockets for untoward or unforeseen medical emergencies which pushes them further towards poverty.
Evidence shows that medical poverty owing to high OOPE increased from 32.5 million in 1999–2000 to 50.6 million in 2011–12.[13] A research conducted in 2019 examined whether poor people in poorer states end up spending more on health expenses. As per 2014 figures, Assam had the highest percentage of people using public health centre (87%) followed by Odisha (80%), West Bengal (70%), Rajasthan (64%). It showed that states that were economically better-off used more of the private health centers, while poorer states used more of the public health centers. Further it also found that the poor in State with higher poverty level used public health services for hospitalisation.
Oxygen shortage
The current stage of the Covid crisis in the country is where people are dying of lack of beds and shortage in oxygen supply. Thus, it is important to look at these parameters before declaring any that any state has performed better than others. Until May 12, Kerala, Tamil Nadu had not raised an SOS for oxygen but on May 13, these states, in addition to Andhra Pradesh raised an alarm to the Centre demanding more oxygen. Kerala which had been sending surplus medical oxygen to neighbouring state Tamil Nadu and Andhra Pradesh, has now halted the supply citing demand in its own state. Officials in Kerala said they had to stop supply to ensure the state is able to meet its own demand, with its Covid caseload expected to rise to 6 lakh by 15 May.[14]
In Conclusion
While these states have fared relatively better than the rest of the states in managing the crisis, it is certainly too soon to laud their efforts. With experts predicting a third wave of Covid to be on its way in India, it is necessary that all states remain on their toes and are consistently keeping up the work they have been doing until and also take lessons from the better performing states such as Kerala, Tamil Nadu and West Bengal so that concerted efforts conclude in a successful stint at combating Covid.
*Feature image by Javed Anees (District Hospital, Tirur) via Wikimedia Commons.
Also read:
Right to Health: The forgotten Constitutional Mandate
References:
[1]https://www.thehindubusinessline.com/opinion/states-that-spend-more-on-healthcare-less-affected-by-Covid/article31738995.ece
[2]https://improvingphc.org/promising-practices/kerala
[3]https://www.aljazeera.com/news/2021/5/11/how-indias-tamil-nadu-and-kerala-states-are-managing-Covid-surge
[4]https://www.thehindubusinessline.com/news/national/how-kerala-became-an-oxygen-surplus-state-in-one-year/article34452802.ece
[5]http://www.swaniti.com/wp-content/uploads/2015/03/Swaniti_Note-on-TN-Public-Health-System.pdf
[6]Dash, A., Mohanty, S.K. Do poor people in the poorer states pay more for healthcare in India?. BMC Public Health 19, 1020 (2019). https://doi.org/10.1186/s12889-019-7342-8
[7]Mukhopadhyay I, Madras T, Madras T. Tamil Nadu state health account 2013–14. 2017. [https://www.researchgate.net/publication/317493240_TAMIL_NADU_STATE_HEALTH_ACCOUNTS_2013-14].
[8]https://www.aljazeera.com/news/2021/5/11/how-indias-tamil-nadu-and-kerala-states-are-managing-Covid-surge
[9] As per NITI Aayog India Index Baseline Report 2018
[10] Closing the health and nutrition gap in Odisha, India: A case study of how transforming the health system is achieving greater equity, Social Science & Medicine, Volume 145, 2015
[11] Closing the health and nutrition gap in Odisha, India: A case study of how transforming the health system is achieving greater equity, Social Science & Medicine, Volume 145, 2015
[12]Sahoo, Niranjan, and Manas Ranjan Kar. “Evaluating Odisha’s COVID-19 response: from quiet confidence to a slippery road.” Journal of Social and Economic Development, 1–15. 25 Nov. 2020
[13]https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-019-7342-8
[14]https://theprint.in/health/tn-andhra-sos-to-pm-keralas-surplus-stock-over-oxygen-shortage-now-hits-south-india/657463/










